Fundamental triple aim of healthcare8/18/2023 In order to achieve a balance in the anticoagulation management literature that supports all three preconditions for the Triple Aim, a further examination of equity in access and quality of care is required. The final Triple Aim precondition that is grounded in equitable care for all, however, remains the least well studied. 7– 8 This research has demonstrated that oral anticoagulants are highly efficacious for patients with conditions such as valvular heart disease, atrial fibrillation, and venous thrombo‐embolism. 4– 6 A second stream of research has focused on defining the appropriate patient population for oral anticoagulation therapy based on specific clinical needs. A considerable body of research has focused on optimal ‘integrative’ models for oral anticoagulant management, by exploring cost effectiveness, quality of care, and patient outcomes for anticoagulation services in physician offices, in dedicated anticoagulation clinics, and in patient self management. The literature, however, remains somewhat unbalanced in favor of the first two preconditions while leaving the issue of equity relatively unexplored. Over the last decade, these three Triple Aim preconditions-the role of the successful integrator, the defined population, and equitable care-have been examined in the anticoagulation therapy and management research. 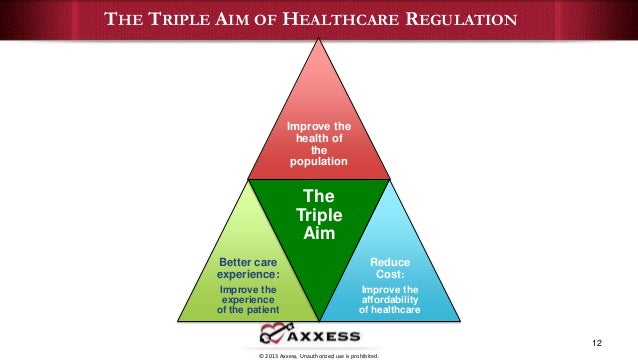
It is the fundamental goal of equity that becomes a lens for understanding quality and access to care to ensure the optimal patient experience. Third, Berwick et al 1 suggested that budget constraints and clear policy levers must be identified that insist upon principles of health equity. As Berwick et al 1 pointed out, “a population need not be geographic” instead a population or subpopulation is often best defined as a group of individuals with a specific set of needs that must be addressed in order to provide the highest quality care. Second, the population of concern must be defined. First, Berwick et al 1 called upon the need for the “existence of an ‘integrator’, able to focus and coordinate services to help the population on all three dimensions at once.” A successful integrator is positioned within the healthcare system to help make connections between communities and their community resources, between patients and their providers of care, and amongst insular health organizations to ensure a successful continuum of care. 2– 3 To provide guidance to organizations pursing the balanced Triple Aim approach, Berwick et al 1 identified three preconditions for success. Since 2008, a groundswell of health organizations in the United States and Canada have been taking up the vision of the Triple Aim with increasing momentum. 2 Is it truly feasible to reduce costs while improving the patient care experience? Can we move away from the deeply ingrained biomedical model to an evolved one that espouses the principles of population health and health equity? 1 Since its inception, this balanced approach to health and healthcare has been a source of debate, striking a nerve amongst healthcare leaders, clinicians providing care, and the patients whose healthcare needs must be met. The framework articulates a set of goals in which health system costs and healthcare quality must be balanced against the needs of the population and improved health outcomes for all. The Institute for Healthcare Improvement's Triple Aim Framework has been gaining ground since its launch in 2008 as an innovative vision for health system reform.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
